"37 little things which have all caused death"

Podcast episode
I've started reading "Essays on the first hundred years of Anaesthesia" by Dr William Stanley Sykes, and thought I'd write a few summary posts highlighting the key takeaway points, both for my own learning, and hopefully for your enjoyment as well.
You never know, they may even be vaguely useful as well.
The first chapter is entitled "Thirty-seven little things which have all caused death", which seems like a splendid place to start, so here goes.
I have not simply copied the chapter, rather I have compiled my own report of the more salient points from which I gleaned either entertainment or new information that I thought the reader might find useful.
Clover's chloroform apparatus
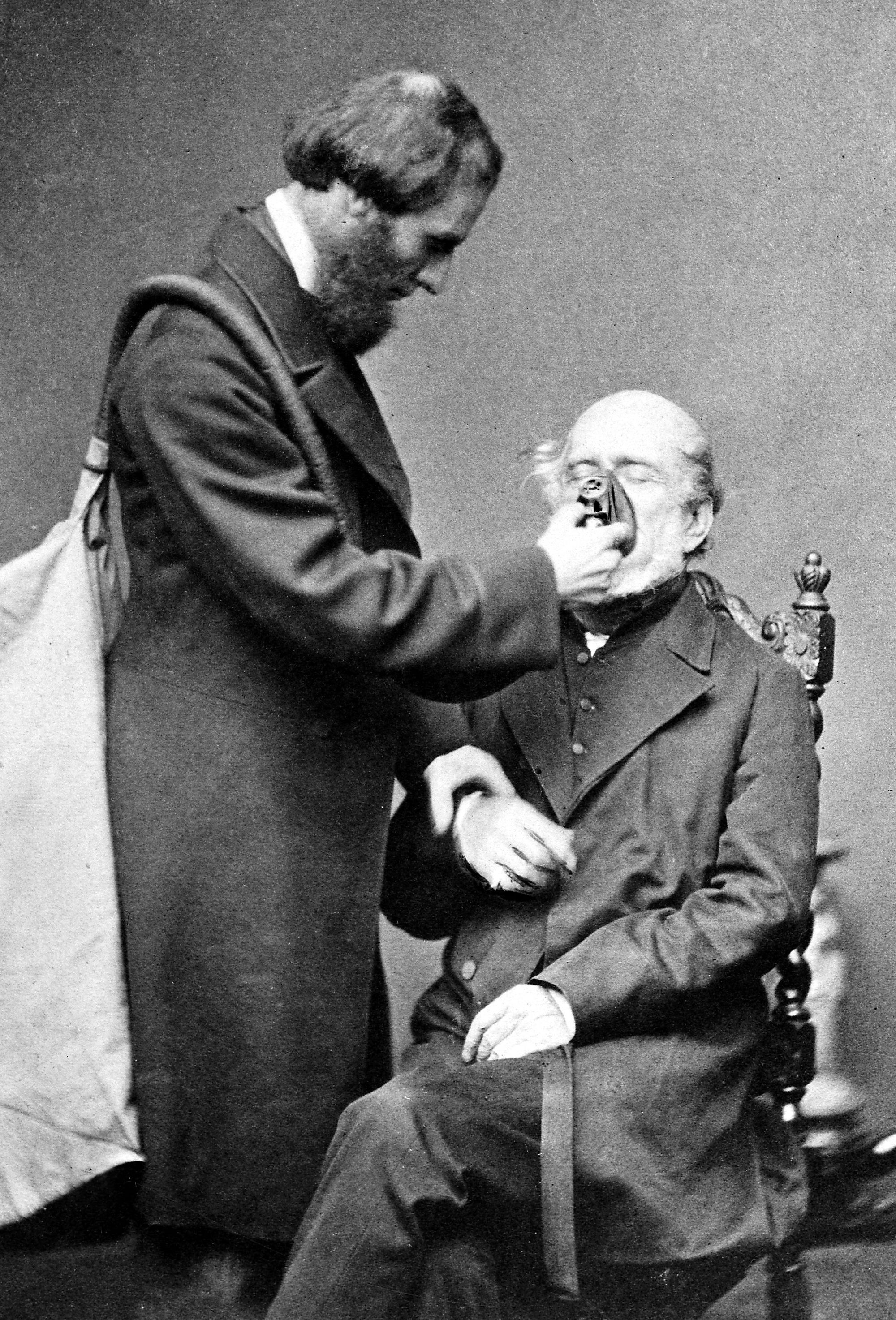
Clover's chloroform apparatus was supposed to make it impossible to administer an overdose of chloroform, however it was a cumbersome and clunky piece of equipment. Featuring an enormous sixteen litre bag with a desired 2.8 percent concentration of chloroform in room air, the idea was that you couldn't ever give too much, because it was already pre-diluted.
However it somehow killed at least one poor patient in 1873, whereupon it was found the bags varied greatly in their true volume, meaning the concentrations delivered frequently varied as high as 3.5%, which proved to be fatal in these cases.
The candle problem
If your surgeon complains too frequently about the operating lights not being in quite the right position, it is humbling to remember the original days of chloroform and ether began by candlelight.
The rather startling problem is that if you bring the candle too close to your chloroform it rapidly denatures and loses its potency, as well as producing phosgene, which is bad news.
"Mey, of Herne, Westphalia, repaired a gunshot wound of the abdomen, evidently a complicated one, for it took four hours. One of the nurses died two days later"
While we sit and complain bitterly that the computer is taking too long to load or the new dexamethasone vials are the wrong colour for our drug tray aesthetic, we would do well to remember a time when anaesthetists had the 'choice of either poisoning everyone in the room with phosgene or blowing them up with an ether explosion'.
Some arrhythmias
One other fatal side effect of chloroform is the array spectacularly bad arrhythmias seen when it is administered with adrenaline. While any competent anaesthetist would have tended to avoid administering adrenaline, it couldn't be helped when the patient decided to do it all by herself.
Here is a quotation regarding an exquisitely anxious woman undergoing dental anaesthesia:
"She had had chloroform five times before without incident. But this time she had heard of a recent death from chloroform in a dental case, and she was very alarmed."
"How right she was, for she died like a shot rabbit before she was under."
Junker's Inhaler

This was a slightly more modern vaporising device used to administer chloroform, however it had one rather substantial drawback when it came to the matter of human factors.
There was no safeguard against connecting the tubes the wrong way round. It was also handed to anyone with a pair of hands and the ability to squeeze the bellows, regardless of whether they actually knew what they were doing.
On more than one occasion - and well into the 20th century - there were occasions whether the entirety of the liquid chloroform was merrily squeezed into the patient's lungs, with the inevitable consequence that is to be expected.
It was only in 1892, when Frederic Hewitt decided to change the tube sizes to make sure they couldn't be connected the wrong way round, that any major advance in safety was seen with this apparatus.
Which leads us to number 3.
Fires and Explosions
The following quote from the aforementioned book, concerns Thomas Nunneley of Leeds in 1849:
"A very large and powerful old male cat was put into a jar with a drachm of oleum aethereum and covered over. It was very late at night, and only one candle left burning. As the light was not very good, in three minutes the cover was removed, and the candle brought near to ascertain the effects; he was seen to be crouched down, soundly asleep; but inadvertently in examining, the candle was brought too near, the vapour became inflamed, and in an instant the whole jar was in a fearful blaze, the cat being completely enveloped in it. The only means to extinguish it was to exclude the air by putting on the cover; this was done; and the flame very soon went out, when the cat was still soundly asleep, not having stirred, being altogether unconsicious of the fire..."
I'm not sure what the MACflame value for oleum aethereum is, but clearly this was an adequate anaesthetic. Kudos to Dr Nunneley.
It appeared that candles and ether gave an interesting combination, and in 1931 there was a spectacularly dramatic case of an explosion in the patient's mouth. The author was at least generous enough to divulge the autopsy findings of 'ruptured bronchi and lung collapse'.
Let's put a candle on the anaesthetic machine.
Yes, you read that right. Behold the early Boyle's gas oxygen machine introduced in 1917:

This nifty bit of kit had a key problem when it came to using nitrous oxide, because the nitrous had just enough water in it to freeze the valves shut in the machine once the nitrous had been in use for any length of time, thanks to our good old friend, the latent heat of vaporisation.
So the obvious answer here is clearly to install a spirit lamp on the machine with the flame delicately licking the affected valves to keep them all toasty and warm. Even better, let's ensure the ether bottle is above the lamp on the same machine.
Enter Murphy and his most ubiquitous law.
A more relevant risk.
When you rapidly compress a gas, the energy that was previously spread out over a larger volume is compressed too, producing a lot of local heat. It is very much the opposite process to that seen when a compressed gas cools as it is allowed to expand.
This process is so reliable at creating conditions that facilitate combustion that it is the essential underlying mechanism for the common diesel combustion engine.
In 1931 a chap by the name of Phillips recorded a fire due to an oxygen cylinder opening too quickly, suddly compressing the air between the valves and allowing a greasy washer to catch alight.
This is why the pressure reducing valve needs to be opened first, the cylinder opened slowly, and care taken to avoid oil and grease contamination of the equipment.
And that, is examinable in the Primary FRCA.
A final point on explosions.
The author Sykes reports himself having come close to witness an anaesthetic explosion when a pesky gynaecologist 'casually leaned on a 750 gallon ethylene cylinder with a lighted cigarette in his hand'. Thankfully the cylinder was closed.
The wrong gas
It seems somewhat obvious that if the wrong cylinder is employed in place of oxygen then the risk of death increases rather substantially, however despite this at least two patients died in 1940 as a result of CO2 cylinders being inadvertently attached to the apparatus instead of oxygen.
Apparently an overly enthusiastic orderly, hoping to leave a good impression at an upcoming inspection, had mistakenly painted the cylinders the wrong colour, 'thereby sentencing two of his comrades to death'.
The Lancet helpfully remarked in 1945 that 'these deaths must stop' and introduced the idea that it should be impossible to connect the wrong gas cylinder to the anaesthetic machine.
This then led to the introduction of the pin index system in 1954, and eventually all of the other cylinder safety features we know so well today.
Spinal Infection
Throughout the history of spinal anaesthesia there have been multiple cases of fatal infections resulting from contamination of the spinal cord and the disastrous sepsis that ensued.
Given the lengths we go to as anaesthetists today to prevent such catastrophes, with our gowning and cleaning and spraying the back with chlorhexidine, it seems downright barbaric that the early practitioners were simply washing the needle and maybe wafting a flame near it as an extra courtesy.
Many of these fatal cases occurred as a result of poor sterile technique or contaminated vials of local anaesthetic agent as one might expect. While his contemporaries set about advising a variety of combinations of boiling, cleaning, towelling and different techniques for safely handling the equipment, D. W. C. Northfield decided that it was the being wet that was the problem, and stated boldly that spinal anaesthesia should be performed dry and with a strict non-touch technique.
Apparently this worked well for the lumbar punctures on his neurosurgical unit, however there isn't a whole load of data to tell us whether he was actually right or not.
Blood transfusion
It's not unheard of for the recipient of a blood transfusion to suffer a devastating fatal complication, despite our best efforts to reduce the inherent risks.
However it's rare for the donor to die.
In the not-so-fab old days a rotary pump was employed to move blood either into or out of the human body. Much like the spinning pumps on the front of the dialysis machines that colonise the intensive care units of today, this hand-driven (then electric) pump from 1888 would squeeze rollers against pliable rubber tubing to push the blood along like a toothpaste tube.
Unfortunately on one disastrous occasion, the safety valve was out of action and the pump ended up working in reverse due to a an inherent circuitry design flaw in the motor itself, causing a fatal venous air embolism to the donor, as all of the drained blood and preceding air was promptly shoved back into his arm.
A rather less surprising venous air embolism, this time delivered to the recipient, occurred after a transfusion was left unattended.
This is of course, bad in its own right, however it gets worse.
The blood to be transfused sat in an inverted bottle above the height of the patient, which sounds moderately reasonable. However we anaesthetists are reknowned for being somewhat impatient, and so they had decided to speed things along with the added feature of compressed air.
This air, sat above the fluid, and supplied by a rubber bulb was guesstimated to take at least forty minutes for the transfusion to finish. So the doctor wandered off for a while.
Enter Murphy's law once again
Of course the transfusion took far less time than expected, and the unintended prescription of 'a whole bunch of compressed air IV PRN' killed the patient rather swiftly.
Other somewhat more forgivable events involved air being sucked in through not-quite-airtight piping, which resulted in the invention of the air trap, which we see in our fluid warming infusion kits today.
Aspiration
It is well established that a full stomach with or without the presence of bowel obstruction is terrifically bad news for the anaesthetist, and has subsequently led to the development of techniques such Rapid Sequence Induction to reduce the risk of gastric contents being aspirated into the respiratory tree.
Interestingly, A. Wilfrid Adams tried his hand at using spinal anaesthesia in an attempt to maintain the patient's consciousness and thereby avoid the risk of regurgitation and aspiration, however despite a satisfactory block to T6,
"The patient drowned in his own vomit"
It is thought the inability to cough effectively as a result of the abdominal wall paralysis somewhat unravelled any benefit of maintaining consciousness, and simply added to the patient's distress.
Lung Abscess
It can be catastrophic if a lung abscess bursts and the contents track across to the healthy lung, hence we have the use of double lumen tubes, and if you're studying for the Final FRCA, then one bulletproof indication for a double lumen tube is lung abscess or pulmonary lavage.
Dr Sykes mentions his own experience of anaesthetising a patient with a lung abscess using the relatively newly employed cyclopropane, sometime after 1933 when it was introduced.
"That patient died on the table, his sound lung flooded by the contents of the abscess."
Even when he tried local anaesthesia to protect the airway reflexes and consciousness, the same thing happened and another patient died. It was only when working in a prison camp in East Germany during the war that he figured out that a steep enough head-down tilt would prevent transfer of abscess contents from one lung to the other, instead allowing the purulent juice to drain cranially instead. He remarks of the intense angle required to facilitate this:
"Forty five degrees is a lot steeper than the steepest gradient on a very severe hill."
Apparently it worked well, with a 'flood of pus' draining out of the nasopharynx rather than into the other lung, and the patient survived.
A Nasal Tube
This is a Magill's tube.

It is a flexible, thin-walled rubber tube inserted nasally using a blind technique, relying on the natural anatomy of the nasopharynx to guide the tube into the trachea.
If inserted through the mouth, however, the more acute nature of the angle between oropharynx and larynx meant the tube was prone to kinking, and at least one unfortunate patient died through 'strangulation'.
And finally - the Epiglottis
The last cause of death that Dr Sykes mentions is asphyxiation as a result of airway obstruction due to the epiglottis being impacted down over the glottic opening, usually as a result of a throat pack being inserted too vigorously.
In one quotation he says:
"Soon after the gag had been placed in position, respiration ceased. I suggested a digital examination. I found the epiglottis impacted in the larynx, and on this occasion, on being picked up, it flew out with an audible click."
As one might expect, the risk of this occurring is highest when the lungs are empty, as the 'relative' vacuum in the chest can suck the epiglottis down making it very difficult to retrieve.
Hence it's a good idea to extubate at full inspiration...
So there you have it, some notes from Chapter 1 of Dr Sykes' 'Essays on the First Hundred Years of Anaesthesia'. Please join us next time as we continue our journey through the veritable jungle that is the history of our wonderful profession.