When to extubate?

Much like flying a plane, the more interesting - and riskier - parts of anaesthesia are generally take off (intubation) and landing (extubation).
Granted there's the occasional in-flight turbulence or unexpected medical emergency to anticipate and respond to, but once you're at cruising altitude you can generally sit down and relax at least a little until it's time to wake up. (The patient, not you).
So the crucial question is - when do I pull the tube?
There are only two reasons to intubate
If you think about every intubated patient that you've ever seen, hopefully they have a purpose-built tube sat snugly between their cords for one or both of the following reasons:
- Airway protection
- Work of breathing
Every indication for every intubation ever boils down to these factors, whether it's an elective laparoscopic cholecystectomy or a head injury patient with a GCS of 4 and evidence of aspiration in the emergency department needing transfer to a tertiary centre - it's still just these two reasons.
So it makes logical sense then, when it comes to removing said tube, we need to ensure both of these parameters are satisfied:
- The patient is going to breathe independently (and adequately)
- They're also going to protect their airway
Preparing for landing
We get nervous about intubating patients, because it's a big deal.
It's viscerally emotive taking someone you probably met less than an hour ago and rendering them dependent on life support, and so we have all sorts of checklists, back-up equipment and spare syringes at the ready to ensure we get it right.
But the other end of the procedure tends to be less choreographed, and certainly less feared by junior anaesthetists, largely because there's usually a sense of enormous relief at having successfully intubated and made it thus far through the operation, meaning the act of extubating the patient can often be dismissed as the 'small remaining step' - which can end up causing issues.
Extubation deserves all the reverence and planning that intubation is given, especially since NAP4 revealed the shocking statistic that around 30% of airway problems occur at the other end of the operation.
The reason that extubation is risky is largely due to an essentially uncontrolled transition from an anaesthetised patient with no (or very little) airway reflex activity, to a fully awake patient with a protected airway, via a wide chasm of 'semi-anaesthetised with exaggerated airway reflexes' in the middle, laced with a variety of -spasms lurking in the depths waiting to pounce.
You know, just to keep life interesting.
Add in to the mix the fact that the surgeon and theatre team are in 'get theatre ready for the next one' or 'get ready to go home' mode - leaving the ODP and anaesthetist to go it alone - and it's easy to see how extubation ends up being the neglected twin of the two most important procedures we do as anaesthetists.
What are the possible complications at extubation?
As always, you should categorise this answer:
Airway complications
- Obstruction
- Coughing and breath holding
- Bucking
- Laryngospasm (around 20%)
- Desaturation
- Vomiting and aspiration
- Bronchospasm
- Inadequate reversal
- Pulmonary oedema*
Traumatic complications
- Mucosal damage
- Dental damage
Cardiovascular complications
- Hypertension
- Tachycardia
- Raised intracranial/intraocular pressure
- Arrhythmias
- Anastomotic bleeding (classically ENT free flaps)
- Myocardial infarction
*Negative pressure pulmonary oedema occurs when a patient in full blown laryngospasm attempts to take a big breath in, generating negative hydrostatic pressure in the thorax and dragging fluid into the alveoli. Bad news.
To continue our aeronautical analogy ad nauseam - you should be fully ready to do a 'go-around' and resedate and reintubate if required.
This means having the kit, the drugs and the people available to achieve said task should you suddenly change the plan at the last minute.
Do you routinely check where your nearest syringe of propofol is before you yank the tube?
Intubation isn't always an elective procedure, but extubation is
It's easy to assume that because you put a tube in at the start, it is therefore your job to take it out again at the end, and that's true for the majority of cases, but it's not guaranteed. There are plenty of operations, both emergency and elective, where you might find it a better option to keep the patient intubated for some time after the procedure, and get in contact with your friendly neighbourhood ICU docs:
Some benefits of delayed extubation on ICU
- Pain control
- Respiratory support
- Airway swelling
- Post operative care after suspected allergic reaction or other critical incident
- To remain intubated prior to re-look operation
Awake extubation
This is taught as the 'gold standard' way to remove a tube from a patient's airway, and when thinking about airway protection and conscious level, it usually is the safest way to do so.
The logic is simple - you wait until they're so annoyed at the tube that they essentially start trying to take it out themselves, whereupon you tell them everything is fine and whip it out safe in the knowledge that your two indications for putting the tube in have thoroughly reversed themselves.
What are the steps to a safe awake extubation?
- Preoxygenate
- Suction pharynx
- Insert bite block
- Position the patient, head up in a suitable position for intubation if needed
- Ensure adequate muscle relaxant reversal
- Ensure patient breathing regular, adequate tidal volumes with minimal support
- Avoid or minimise movements of the head and neck
- Wait until eyes open and obeying commands
- Apply positive pressure to recruit the lungs
- Deflate the cuff slowly
- Remove the tube
- Apply facemask and confirm ventilation with end tidal CO2
However as you may have noticed it's not all that much fun having a lump of plastic between the vocal cords, and patients can look very uncomfortable during those final wake up moments, even if they don't remember a thing later on.
Aside from being uncomfortable, this coughing and bucking can be disastrous for the surgeon if it disrupts all of the hard work they've just put in by causing surges in pressure and muscle tension around delicate suture lines and blood vessels.
Key examples are:
- Neurosurgery
- Ophthalmic surgery
- ENT
- Plastics
How to avoid coughing on the tube
- Small doses of rapid acting opioid
- Lidocaine (IV, sprayed onto the cords or in the tube cuff*)
- Propofol
- Ketamine
- Dexmedetomidine
- Deep extubation
*I've started putting 2 or 3 mls of 2% lidocaine in the cuff for patients that smoke, and very anecdotally have noticed they probably cough a bit less.
An alternative to awake extubation is to do precisely the opposite.
Deep extubation
When done well, deep extubation is a sight to behold - the tube slides out, the patient remains fast asleep, quietly and comfortably breathing as they glide to recovery to wake up in their own time.
No coughing, no bucking, happy patient and happy surgeon.
It can be very useful in patients with asthma or recent chest infection who are at substantially higher risk of developing bronchospasm and laryngospasm at extubation.
Extubating deep has several benefits
- Reduced coughing and bucking
- Reduced surges in blood pressure
- Reduced surges in intracranial pressure
- Less strain on abdominal wounds
- More comfortable wake up
It has been thought in the past that waking up sans-tube causes less emergence agitation but the evidence suggests that the incidence of emergence agitation isn't affected by awake vs deep extubation.
The key to deep extubation - as with everything we do in anaesthesia - is to plan it properly, and to use it in the right cohort of patients.
Who should you not deep extubate?
- High risk of aspiration (emergency or abdominal procedures)
- Likely to be difficult to reintubate or facemask ventilate
- High risk of airway obstruction unless wide awake
- Any patient that you're anaesthetising on your own as a junior
Ensure they're deep enough
In the same way you'll run into trouble trying to extubate a patient that's not awake enough, you'll find similar peril in trying to extubate a patient that isn't deep enough either.
Avoid the second plane of anaesthesia - extubate in plane 1 (awake) or 3 (surgical anaesthesia)
The steps to safe deep extubation
- Ensure you have the right sort of patient (and anaesthetist)
- Check for haemodynamic stability
- Ensure fully reversed muscle relaxation
- Ensure at least 1 MAC or equivalent depth of anaesthesia
- Thorough suctioning of pharynx
- Establish spontaneous ventilation with sats >95% and tidal volumes >5ml/kg without significant support
- Preoxygenate with 100% FiO2
- Slowly deflate the tube cuff, and check for breath holding (suggests too light to deep extubate)
- Remove tube
- Ensure regular spontaneous breathing re-established
- Discontinue administration of anaesthetic agent
- Monitor very closely until awake
When should I give the reversal?
Before you need them to be breathing by themselves.
Classical reversal with neostigmine and glycopyrrolate generally takes at least a few minutes to work, but with the luxury of sugammadex you can slam that roc into oblivion in a matter of seconds, which you can use to your advantage.
Given you're reading this, and sugammadex is now off patent - I'm going to go out on a limb and assume you're familiar with its use.
For a deep extubation, you need to give the reversal early, to establish solid spontaneous breathing before you then proceed to take the tube out, otherwise as you can probably imagine your extubation is likely to be suboptimal.
You can of course do the same for an awake extubation - which many anaesthetists do - and give the reversal nice and early on to establish spontaneous breathing before the operation has finished. This is fine, and certainly safe, because it reassures you that the patient is breathing well enough to extubate at the end.
However for an awake extubation you can be a little more artistic.
A paralysed patient won't cough or buck on the tube, which is handy when sliding them across onto the bed after the procedure, and when doing that last-minute airway suctioning you forgot to do while they still had a load of anaesthetic agent on board.
Because sugammadex works so quickly, you can give it once your patient is comfortably and safely positioned in the bed and pretty much ready to wake up.
What about awareness?
Many people worry that if they give the sugammadex too late then the patient will be paralysed and awake and enormously distressed by the whole situation, and in theory this is a possibility.
However consider the fact they have just had an operation, they've likely got at least forty-five minutes' worth of anaesthesia and strong opioid analgesia swilling around in their system, and they may well have started taking little breaths by themselves already.
Ask any patient who's had an (adequately anaesthetised) operation what they remember and they'll usually start from being in recovery, or even back on the ward.
If you're giving the reversal with a matter of minutes of their MAC being low enough to risk awareness - and they haven't got a blood pressure and heart rate suggestive of significant distress - chances are they're not going to be bothered in the slightest by being slightly weaker than usual, if they're even aware of it at all in the first place.
A Quick bit about laryngospasm
Laryngospasm occurs when annoyed vocal cords go into protest by slamming shut and preventing anything from getting past, including oxygen, which winds up the recovery staff no end if you don't fix it fairly promptly.
Laryngospasm usually occurs when the patient is in plane 2 of anaesthesia (that turbulent bit in the clouds before you see the runway below) and there are bits of blood or secretions tickling the top of the vocal cords.
Now in theory, because they are controlled by a muscle, the vocal cords will not be able to sustain this spasm to the point of seriously dangerous hypoxia because the muscle will become too hypoxic to maintain sufficient tone before the brain becomes starved of vitamin O.
But this isn't a theory we tend to test.
Laryngospasm is best avoided, and second-best treated fairly swiftly.
How to avoid laryngospasm
- Get any airway manipulation done while the patient is deeply asleep or still relaxed (assessing view, suctioning secretions, airway exchange etc)
- Ensure thorough clearance of secretions, blood and other soiling before extubation
- Minimise head and neck movement when transferring to the bed and when patient is waking up
- Deep extubation when appropriate
How to manage laryngospasm
- Remain calm and avoid stimulating the larynx any further
- Apply PEEP up to 30-40cmH2O with 100% oxygen via a facemask
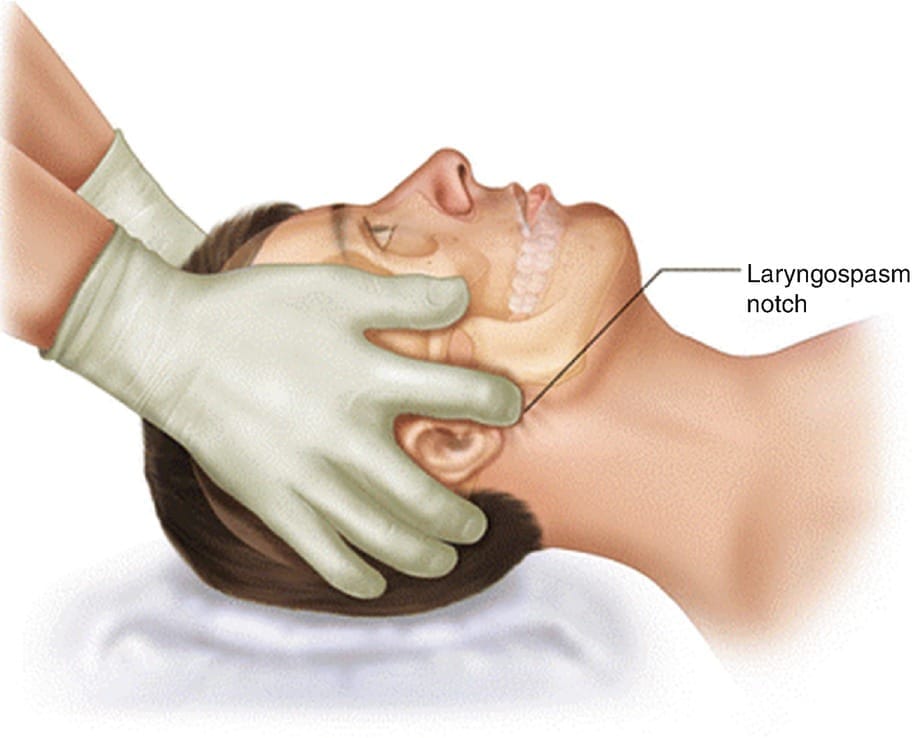
- Larson's Manoeuvre*
- Resedate if required
- Reparalyse if required
*Press very firmly with the middle fingers into the space immediately behind the lobule of the pinna of the ear (anterior to mastoid process) while doing a gentle jaw thrust.
It works well enough that Dr Larson called it The best treatment for laryngospasm.
Check out our full post on laryngospasm here
Useful Tweets and Resources

Do you extubate children awake or deep?
— British Journal of Anaesthesia (@BJAJournals) February 17, 2022
Although awake extubation may seem like the safer option, it is not necessarily appropriate in all situations and increases the risk of adverse reflexes such as coughinghttps://t.co/01gPhT2AS0 #anaesthesia #paedsanaes #BJAEducation pic.twitter.com/ijlqpbzwow
References and Further Reading


Members Area
FRCA Questions
