Rheumatoid Arthritis
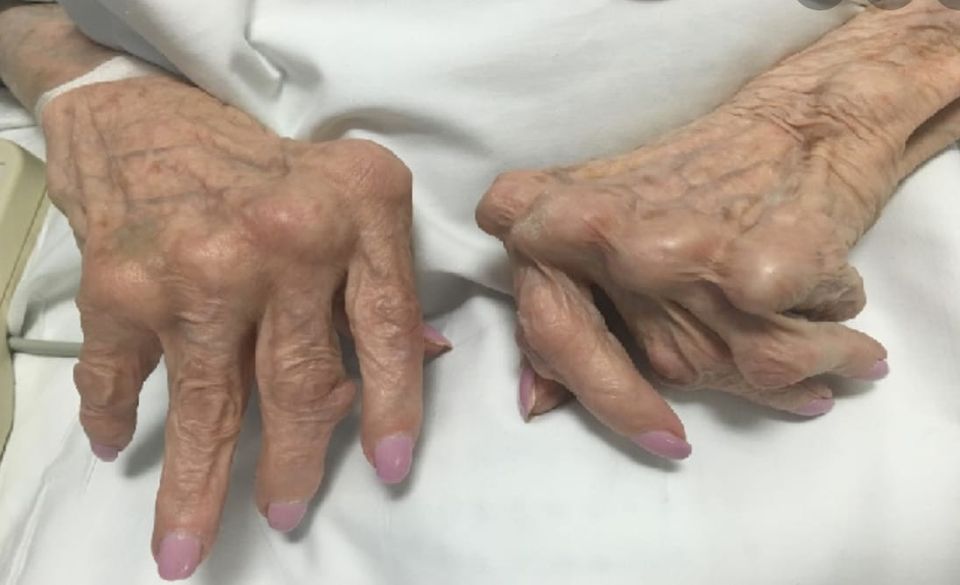
A rapid revision post for the Final FRCA examinations, with all the highest yield questions for the CRQ and SOE components.
A 52 year old man with a history of rheumatoid arthritis is undergoing a right-sided inguinal hernia repair.
Explain how you would assess this man's airway
As always, structure your response by stating you would take a thorough history and perform a focused examination followed by relevant investigations and imaging.
History
- Previous airway documentation or difficulty
- Symptoms including joint pain and stiffness
- Particularly ask about neck pain and stiffness, and evidence of upper limb neurological symptoms such as paraesthesia*
- Ask about shortness of breath and hoarseness that may indicate cricoarytenoid pathology
- Dental history
*Overenthusiastic airway manipulation + atlanto-axial instability = paralysis or death
Examination
- General factors that predict difficult airway
- Mouth opening
- Neck movement
- Jaw protrusion
- Mallampati
- Thyromental distance (<6cm is concerning)
- Sternomental distance (<12.5cm is concerning)
- Wilson score
Investigations
- C spine xray
- MRI if any concern on C spine xray
- FNE (flexible nasendoscopy) to assess for laryngeal pathology if concerned
What is the Wilson Score?
Five factors that are indicative of a difficult intubation.
- BMI
- Jaw protrusion
- Neck mobility
- Receding mandible
- Buck teeth
>1 risk factor has a sensitivity of 75% and a specificity of around 88% for difficult intubation
What is rheumatoid arthritis?
- A chronic systemic inflammatory autoimmune arthropathy
- Causes symmetrical cartilage loss and bony erosion
- Can also cause tenosynovitis and extra-articular manifestations
What's the prevalence?
- 0.5 - 1% of the Western population
- 3:1 female to male ratio
- Peaks at 30 - 55 years
What causes it?
- We usually don't know the exact trigger
- Around 70% of cases are associated with the HLA-DR4 subtype
- 80% of patients are seropositive for Rheumatoid factor
- Anti-CCP antibodies are more specific
Risk factors:
- Smoking
- HLA-DR4 phenotype
- Female sex
- Family history of RA
- Atopic phenotype
- Altered gut flora
- Stress
- Heavy metal exposure
Anything that might kickstart an already twitchy immune system.
What are the clinical features?
In the exam they might ask you for signs or symptoms, and you won't score any points if you list from the wrong category.
Symptoms
- Symmetrical joint pain worse in the morning and improving with activity
- Stiffness, again worse in the morning
- Fatigue
- Weight loss
- Malaise
- Low mood
Signs
- Tender, warm joints
- Soft tissue swelling
- Limitation of movement
- Deformity
- Nodules
Which joints are most commonly affected?
- Fingers and toes
- Wrists and ankles
- Elbows and knees
- Shoulders and hips
- Neck
What's the prognosis?
- Highly variable with a range of pattern and progression
- Depends on treatment and response
- Also depends on the extent of extra-articular manifestations
Rheumatoid arthritis may significantly reduce life expectancy, particularly with severe disease and extra-articular involvement.
What are the symptoms of cervical subluxation?
- Pain radiating to occiput
- Paraesthesia
- Sudden weakness in hands
- Sensory loss
- Gait abnormality
- Urinary incontinence or retention
Atlantoaxial subluxation occurs in up to 25% of patients with severe rheumatoid arthritis.
What are your anaesthetic concerns specific to the musculoskeletal features of rheumatoid arthritis?
They're asking this because they want you to say something other than cardiac or respiratory issues.
- Temporomandibular joint dysfunction can reduce mouth opening and make intubation more difficult
- Cricoarytenoid joint involvement can cause hoarseness or stridor and increase the risk of postoperative airway obstruction
- Spinal involvement can reduce neck extension or increase risk of spinal cord damage during airway manipulation
- Manual dexterity is needed to operate a PCA button
Why might their airway be challenging?
- Atlanto-axial subluxation* - spinal cord compression, vertebral artery compression
- Neck stiffness - difficulty positioning for intubation
- Glottic stenosis - amyloidosis, rheumatoid nodules
- Cricoarytenoid joint dysfunction
- Temporomandibular joint dysfunction - limited mouth opening and jaw protrusion
*Anterior atlanto-axial subluxation is most common and is worsened by flexion.
Posterior or vertical AAS is worsened by extension.
What are the extra-articular manifestations of rheumatoid arthritis that may be of concern to the anaesthetist?
As always, break this down by system, and specifically state why it is of concern to the anaesthetist.
Respiratory
- Restrictive lung disease - fibrosing alveolitis and hypoxia
- Costochondral disease - reduced chest wall compliance
- Pleural effusions - ventilation:perfusion mismatch
Cardiovascular
- Myocarditis, endocarditis and pericarditis - left ventricular failure
- Pericardial effusion - tamponade and reduced cardiac output
- Fibrosis and nodules in conducting system - conduction defects
- Raynaud's phenomenon - poor sats trace
- Increased rates of ischaemic heart disease - perioperative MI risk
- Peripheral vasculitis - risk with TED stockings
Neurological
- Eyes - keratoconjunctivitis, dry eyes and risk of corneal abrasion
- Autonomic neuropathy - intraoperative hypotension
- Peripheral neuropathy - positioning and nerve injury
Renal
- Amyloidosis - reduced drug clearance
- Caution with renal function and long term NSAID use
Musculoskeletal
- Contractures and pain on positioning - risk of nerve injury and pressure points
- Thin skin due to steroids - cannulation and positioning risk
Haematological
- Anaemia - may need transfusion
- Increased risk of VTE
What medication-related effects of rheumatoid arthritis may be of concern to the anaesthetist?
- Steroids - blood sugar control, thin skin, easy bruising
- Immunosuppression
- Deranged LFT
- Renal toxicity
What are the symptomatic treatment options for rheumatoid arthritis?
Break this down into non-pharmacological and pharmacological
Non-pharmacological
- Physiotherapy
- Occupational therapy
- Massage
Pharmacological
- Paracetamol
- NSAIDs
- Steroids for acute flares
- Opioids for chronic pain from joint destruction
Do you know any DMARDs used for rheumatoid arthritis?
- Methotrexate - anti-metabolite
- Sulfasalazine - immunomodulator
- Azathioprine - purine antagonist
- Ciclosporin - calcineurin inhibitor
- Hydroxychloroquine - toll-like receptor antagonist
- Gold - unknown
- Anakinra - IL-1 receptor antagonist
- Leflunomide - pyrimidine antagonist
Do you know any biologics used for rheumatoid arthritis?
Anti-TNF agents:
- Etanercept
- Adalimumab
- Infliximab
Others:
- Rituximab
- Tocilizumab
- Abatacept
What are the key concerns with methotrexate?
- Liver toxicity
- GI toxicity
- Pulmonary fibrosis
- Immunosuppression
- Interaction with other drugs
- Bone marrow suppression
Ciclosporin is nephrotoxic and sulfasalazine can trigger SJS.
What are the consequences of long term steroid therapy?
- Obesity - cardiovascular and respiratory complications, manual handling difficulty
- Hypertension - intraoperative haemodynamic instability
- Thin skin - manual handling, bruising and skin tears, pressure points
- Diabetes - glucose management, poor wound healing, increased MI risk
- Immunosuppression - increased infection risk
- Hypokalaemia - arrhythmia risk
- Osteoporosis - fracture risk
- Adrenal suppression - need for perioperative steroid replacement if ongoing therapy
Outline your preoperative priorities for a patient with rheumatoid arthritis
Break this down into history and examination, investigations and pre-operative optimisation.
History and Examination
- Severity of disease
- Extra-articular features - particularly airway and C spine
- Full airway assessment - neck flexion, TMJ function
Investigations
- Bloods - anaemia, renal involvement, liver dysfunction
- Imaging of the C-spine if any concerning history or examination
- Flexible nasendoscopy - if stridor or vocal changes suggestive of cricoarytenoid joint involvement or glottic stenosis
- CXR - pulmonary toxicity from medications
- Lung function tests - may demonstrate restrictive lung disease
- ECG - conduction abnormality, ventricular strain
- ECHO - if any concern about cardiovascular disease
Pre-operative optimisation
- Correct anaemia
- MDT perioperative management of DMARDs and biologics with rheumatology
- MDT management - frailty, physiotherapy, dieticians
What are your intraoperative priorities?
- Monitoring - AoA as always, consider arterial line if haemodynamic concerns
- Venous access may be difficult with steroid use
- Restricted neck movement may make jugular access for CVC more difficult
- Avoid C-spine manipulation - local/regional anaesthesia, MILS
- Prepare for a difficult airway - consider awake tracheal intubation*
- Supraglottic airway may avoid risks of intubation and cause less laryngeal oedema
- Consider eye drops if indicated
- VTE prophylaxis
- Antibiotics as indicated
- Extra care with sterility of procedures - immunosuppressed
- Caution with positioning - joint pain, pressure points, thin skin
- Steroid management as per guidelines
*This also allows you to monitor neurological symptoms during intubation.
What are your postoperative priorities?
Nothing new here, it's analgesia, anti-emesis and getting them back to their day to day life as quickly as possible.
- Multimodal opioid sparing analgesia - as usual
- Anti-emesis - to facilitate oral intake of usual medications
- Physiotherapy and occupational therapy where needed
- VTE prophylaxis
- Early mobilisation
How would you manage a high risk extubation?
- Only extubate once fully awake
- If any concern, transfer to ITU intubated for delayed and more controlled extubation
- Tracheostomy
- Other airway techniques including - exchange for Igel, airway exchange catheter
Cricoarytenoid disease increases the risk of delayed airway obstruction post-extubation.
References and Further Reading





The Toolkits
Everything you need to smash the exams, all in one place.


