Paediatric Endoscopy
Take home messages
- There's no one right way to anaesthetise a child for endoscopy, but there are plenty of ways to mess it up
- Intubation is probably the best plan if you're in any doubt about the patient or procedure (or endoscopist...)
- Don't forget the gas
An elective paediatric endoscopy list
Today I was placed onto an elective paediatric endoscopy list with three cases, so to consolidate my own knowledge and pass on some tips and tricks, I thought a post might be nice.
So here we go.
The list:
- 9 year old for OGD
- 9 year old for OGD and colonoscopy
- 16 year old for OGD and colonoscopy
In this instance, all three children were generally fit and well with no cardiorespiratory comorbidities or developmental problems, however our poor teenager had been suffering with rather severe Crohn's for a year or so, including the need for infliximab infusions.
What are your anaesthetic concerns for a paediatric endoscopy patient?
- Reflux
- Duration of procedure
- Aspiration risk
- Recent aspiration
- Bowel prep
Reasons kids might need endoscopy
Entire GI tract issues
- IBD
- Chronic pseudo-obstruction
- Polyposis
- Post-transplant lymphoproliferative disease
- Graft vs Host disease
- Blood vessel disorders such as angiodisplasia
Just the top end
- Oesophagitis
- Gastritis
- Ulcers
- Coeliac
- Pyloric obstruction
- Strictures
- Barrett's oesophagus
- Eosinophilic oesophagitis
- Achalasia
- Varices
- Toxic or caustic ingestion
Just the bottom end
- Colitis
- Hirschsprung's disease and other dysmotility issues
- Haemorrhoids and fissures
Other things they might do while they're there
- Injection of adrenaline or botox
- Insertion of tubes
- Banding of varices
- Biopsies and polypectomies
- Balloon dilatation
These are unlikely to be topics that you'll be grilled on in an exam, but it's good to be aware of them as they might add a risk of bleeding or allergic reaction, or the occasional vagal bradycardia just to keep your list interesting.
A quick overview of some of the specific conditions the kids may have:
Paediatric GORD
- Reflux is common and usually goes away by 1 year
- It becomes GORD if it starts causing significant issues or complications
- Usually it's due to the lower oesophageal sphincter relaxing inappropriately but it canx be due to hiatus hernia or other oesophageal disorders
- You will almost certainly get an exam question on congenital hiatus hernia at some point so it's worth giving it a glance over
How to treat GORD
In the unlikely event that you as an anaesthetist are managing paediatric GORD by yourself, here are some options:
- Simple feeding advice, with smaller meals
- Acid inhibition such as proton pump inhibitors
- Smooth muscle relaxation such as baclofen)
- Surgical options include fundoplication
Coeliac disease
Symptoms
- Chronic diarrhoea
- Abdominal distension
- Failure to thrive
- Nutritional deficiencies
- Other immune problems
Associations
- Autoimmune thyroid disease
- Diabetes Mellitus
- Turner syndrome
- Williams syndrome
- Down syndrome
Diagnosis
- Gold standard is positive serology - (IgA) tissue transglutaminase antibodies - plus biopsy
Inflammatory Bowel Disease
- Crohn's and Ulcerative colitis are the most common but others exist
Crohn's
- Can affect any part of the GI tract
- Skip lesions
- Transmural inflammation
- Fistulating and stricturing processes may be present
Ulcerative colitis
- Continuous
- Colon
- Superficial inflammation so doesn't cause strictures or fistulae
Diagnosis
- OGD and Colonoscopy
- Biopsies
- Surveillance may be needed too
Treatment
- Nutritional
- Anti-inflammatories (mesalazine and sulhpasalazine)
- Immunosuppresants (methotrexate and steroids)
- Biologics (Infliximab)
The Final FRCA will ask you how infliximab works (Anti - TNF-α), and will ask you about perioperative considerations for patients with inflammatory bowel disease - so don't forget steroid replacement and anaemia.
Patients on endscopy lists often have allergies or intolerances, which is frequently the reason for the endoscopy in the first place - remember that children with a soy or egg allergy can still have propofol*.
*I imagine there are a lot of people who would agree it's sensible to try something else if a patient has a history of vigorous anaphylaxis to egg.
Specific Anaesthetic Considerations
As always, start your answer with something along the lines of 'comprehensive preoperative assessment with history and examination'
History
- Weight and nutritional status
- Reflux
- Medications including steroids and immunosuppressants
- Long term lines such as Hickman line or PICC line
- Discuss with endoscopist whether they want the patient to have antibiotics
Examination and Investigations
- Bowel prep can cause vomiting and dehydration
- Macrogol is also known to frequently cause hypokalaemia
- Immunosuppressants may require testing such as full blood count and electrolytes preoperatively
Anaesthetic technique
Questions to address when deciding your plan of attack:
- Are you going to protect the airway?
- Are you going to breathe for them?
Option 1: Sedation only with native airway
So apparently, NICE recommends midazolam for OGD and midazolam + fentanyl (or equivalent opioid) for colonoscopy, however the evidence seems to suggest that it's not as good as propofol TCI and has higher risk of complications than general anaesthesia.
This is what we did for our first patient on the list:
- IV cannulation with Ametop
- Lidocaine to numb the vein
- TCI and high flow nasal oxygen
- Propofol titrated up to 3.5 microgram per ml as a target plasma concentration
- 400mcg alfentanil titrated to respiratory rate for the more stimulating parts of the procedure
- High flow nasal oxygen set at 60 litres per minute
The procedure was quick and uneventful, the child remained spontaneously breathing throughout and so as soon as the endoscope was out, we switched of the propofol and swapped the HFNO to a conventional facemask and wandered straight round to recovery.
Fun fact - Apparently some endoscopists find the biomechanics of spontaneous breathing are helpful for colonoscopy.
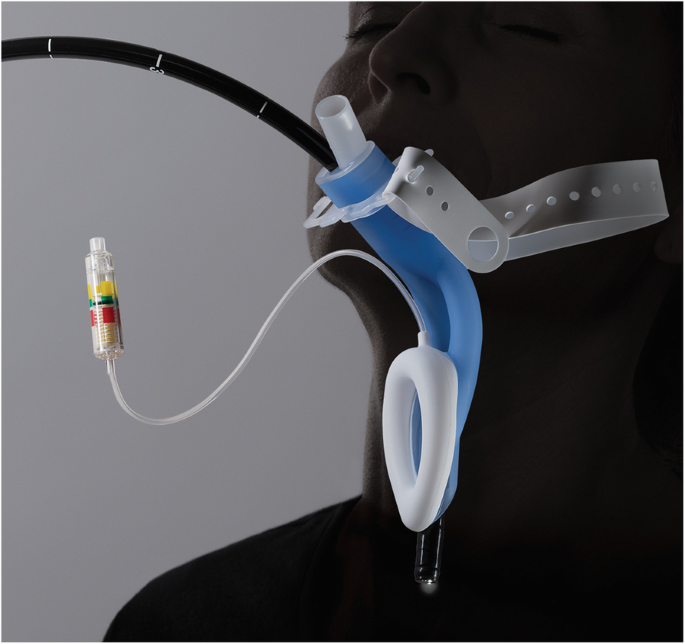
Option 2 - Supraglottic Airway
I've never done it this way myself - I've only ever tubed or used high flow nasal oxygen with sedation - but apparently it works quite well.
Just remember to use a smaller IGEL than you might otherwise have picked.
Interestingly there is also the LMA Gastro that has a dedicated endoscope port, which works moderately well according to many people, but I've never seen it used myself and it's not licensed in children so maybe ignore this bit.
Intubation
By now I'm hoping you're familiar with Anaestheasier's third rule.
While many clinicians will opt to tube when others might not, there are a few scenarios in which you should definitely be thinking of grabbing a laryngoscope:
- If they're less than a year old or really tiny (<10kg) then it's probably best not to mess around, given they desaturate so quickly and SGAs don't tend to sit all that well
- If they're known to have significant airway issues or obstructive sleep apnoea
- Significant cardiac or respiratory co-morbidity is pretty much always an indication for intubation in any patient, (so stick this down in a CRQ if you're struggling for answers)
- High risk of aspiration, including GORD or congenital oesophageal problems
- Some particular procedures (such as PEG tubes) generally need intubation, especially if they're going to take a long time or need multiple position changes for the patient
Because of the length of the procedures and potential need to reposition, we opted to intubate both of our second two patients on this list.
- IV cannulation with Ametop
- Lidocaine to numb the vein
- Preoxygenation with 100% oxygen
- Fentanyl bolus
- Propofol bolus for induction
- Parent allowed to kiss their child and escorted swiftly out at this point
- Rocuronium bolus
- Intubation using direct laryngoscopy and cuffed ET tube
- Wheeled into theatre and positioned in left lateral position
- No need for bite block as paralysis given
- Fentanyl boluses as required
- Sugammadex prior to wake up
Where I work, patients need to be extubated before transfer to recovery, so there was a bit of a delay while we waited for our sleepy little ones to resurface, but it wasn't a high-paced list so the safety of intubation hugely outweighed any downsides.
All three kids were reviewed on the ward afterwards - comfortable, happy and - crucially - blissfully unaware of the morning's events.
Gas problems
No matter how diligently your endoscopist deflates the stomach and oesophagus prior to removing their scope, there will always be air in the stomach when it comes to wake up time.
This can present a number of issues:
- Discomfort and pain
- Nausea and vomiting
- Aspiration risk
- Splinting of abdomen and respiratory compromise
Gently pressing on the abdomen, or event a quick naso- or orogastric tube can help remove some of that air and make your life a little easier.
Useful Tweets
What are the indications for tracheal intubation during endoscopy?#BJAEducation paper on anaesthesia for paediatric GI endoscopy.https://t.co/CsYXMd13jg#PaedsAnaes #PedsAnes
— British Journal of Anaesthesia (@BJAJournals) March 29, 2019
Emergent upper endoscopy performed with pediatric colonoscope for the management of diverticular hemorrhage in the jejunum. @GVAhgandia @Tokioblues2 @ClarsPeiro @alemany_gloria @marilozahonero @escapa79 @TOMASFUSTERBELL pic.twitter.com/wFjdgcssgY
— Lidia Martí (@guanxa_m) May 23, 2022
Not strictly relevant but cool - these clever people managed to get all the way to the jejunum in a bleeding adult using a paediatric colonoscope.
References and Further Reading
- BJA ed - Anaesthesia for children having endoscopy on a gastroenterology list
- https://litfl.com/button-battery-update/
Looking for free CRQs for the FRCA?


