Sedation in ED - a case discussion
The aim of this post
The goal of Anaestheasier is to generate a community amongst our members where we can share tips and tricks and best practice from across the world. As such we thought it might be interesting and useful to go through cases we've seen and break down what happened, what we did and why - for two reasons:
- For our readers to learn what an anaesthetist does in each scenario
- To get feedback on how others feel we could have done better
I've tried to write it in a way that makes it accessible to all, whether you're a student, doctor, anaesthetist, paramedic, nurse, associate practitioner - hopefully it is useful, and please don't hesitate to ask any questions at all - even if it's just to clarify something we've said.
For the medical students
Every medical student I have worked with has said essentially the same thing:
"Anaesthetics is a huge specialty but gets little-to-no attention at medical school."
We have made it our mission to right this wrong.
And for the seasoned anaesthetists among you - let it rip!
Seriously - we want you to critique our management, suggest what we could improve or highlight anything that was just plain wrong - so that we can all become better anaesthetists.
Give us your best shot in the comments!
The Case
An 18 year old male had been walking along a narrow brick wall at a height of around 10ft when his tequila-enhanced cerebellum lost focus and he slid to one side, catching his elbow on the way down and dislocating the ulna posteriorly.
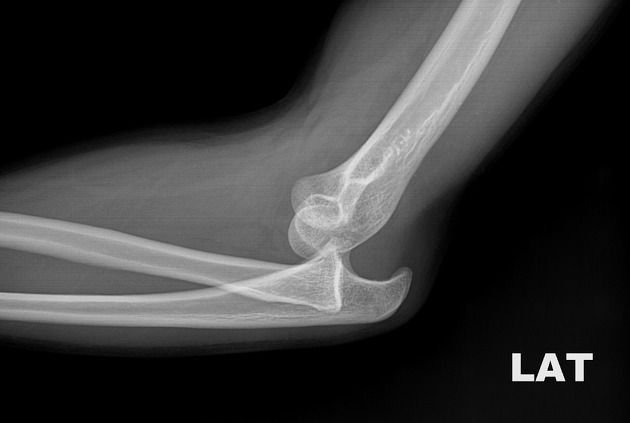
Not the patient's xray - but to the untrained eye it looked the same.
He had an unremarkable primary survery and no other distracting injuries of note, so it's just the elbow that we're concerned about.
Neurovascularly intact but in a lot of pain, he was referred to us for some help with sedation while the orthopaedic registrar attempted to manipulate it back into position.
What is sedation?
Pretty much anything and everything to do with human beings can be viewed on a spectrum, and sedation is no different.
If at one end of the spectrum we have 'wide awake' and at the other end we find 'general anaesthesia', sedation is somewhere in the middle, sliding one way or the other depending on how 'heavy' the sedation is.
What are we aiming for?
- Avoid a general anaesthetic - otherwise we'd just do a GA
- Patient to tolerate a painful but brief procedure and ideally not to remember it
- Patient to remain spontaneously breathing
- Patient to remain cardiovascularly stable
- Patient to protect their airway as much as possible
The most important question to answer is the following:
"If I give this patient sedation, am I putting them at undue risk of cardiovascular or respiratory compromise?"
Respiratory compromise could be direct respiratory depression from the cocktail of magical medicines you're about to flood into the chap's vein, airway obstruction by a vast quanitity of pharyngeal soft tissue, or trouble as a result of aspirating on the three course meal he ingested an hour ago.
Cardiac compromise could be in the form of hypotension from overzealous sedation, or an underlying cardiovascular pathology that has yet gone undetected in the patient's medical journey.
Things to think about
- Fasting status and vomiting
- Comorbidities
- Regular medications
- Allergies
- Problems with previous anaesthetics
- Likelyhood of needing further intervention*
*In younger children especially, the orthopaedic team may manipulate the joint/limb/fracture only to find it now isn't quite as stable as they were previously hoping, and as a result some metalwork +/- hammering may be required, which clearly requires more than 'a bit of sedation'.
If there is any inkling of a possibility that they might need to do more than literally clicking something back into place, then it's vastly safer and more convenient for everyone involved to do it as a proper case on CEPOD under general anaesthesia.
So what did we do?
After a brief chat with the patient (and parent) we were happy that he was well fasted, not vomiting and the procedure was likely to be a quick relocation and application of backslab with no further intervention needed.
I explained the concept of sedation - "It's not a full anaesthetic, it's to make you unaware of what they're doing, so that you're not bothered by it and it doesn't hurt."
I then emphasised to Mum - "It's normal if he moves around a bit or makes some noises while they're moving his arm around - he's not aware of it or in pain, it's just a natural reflex response."
We then cracked out the checklist
Once we were happy sedation was the right answer and we started drawing up our cocktail of choice, one of the ED nurses handed us a conscious sedation checklist.
The Checklist
- Have you got the right patient expecting the right procedure?
- How much do they weigh?
- Have you checked allergies, medications and comorbidities?
- Fasting status
- ASA score
- Who is in charge of doing the procedure?
- Have you got airway equipment and emergency drugs available?
- Have you got working suction ready?
- Have you applied all the necessary monitoring (capnography is key)
- What drugs are you using and how much?
Then for afterwards
- Any immediate issues?
- Any further doses given?
- Any follow up required?
With our estimated 70kg patient positioned comfortably, all the necessary equipment, meds, and checklists sorted, we popped on a capnography mask and gave:
- 70mg ketamine - for sedation and analgesia
- 30mg propofol - to contribute to sedation and to smooth out the emergence
After thirty seconds he was away with the fairies and the orthopods clunked his elbow back to where it should be. The patient's other arm flinched a little at the most stimulating point of the manouevre but otherwise he remained comfortably asleep, and most importantly - spontaneously breathing.
Check the nurses are happy
It's often a bit anticlimactic once the deed is done and the plaster is on. The orthopaedic team wander off to find some other bones to fix and you're left with a sedated patient.
A sedated patient who now has much less pain in their joint providing any form of stimulation, so they usually remain rather sleepy for a while.
They also sometimes stop breathing at this point, hence the capnography mask.
We stuck around until the nurse (and most importantly the parents) were happy that he was on his way back to the real world, comfortable and safe to maintain his own airway and breathing, after which we signed the checklist and headed back out into the night.
What are your options for procedural sedation?
- Propofol (1 mg/kg)
- Propofol + fast acting opioid (TCI infusion or boluses)
- Ketamine (1 mg/kg)
- Ketofol
- Midazolam (0.02 mg/kg)
- Fentanyl (1 mcg/kg)
Any reasonably sensible combination of the above agents is acceptable, and of course there are other less commonly-used options as well such as dexmedetomidine - the key is to practice and get comfortable with your way of doing it, and stick to it.
Remember to adjust your dose to the patient in front of you - as a general rule if the patient is elderly and frail you should halve the dose.
ish.
Oral, nasal, IM or IV?
This usually applies more to kids than adults, generally as a result of refusal to allow a cannula to be inserted, however occasionally you might find yourself in front of an adult needing an alternative method of administration, and usually rather pronto.
Ketamine is a magical medicine, inducing a unique form of dissociative anaesthesia by essentially telling the thalamus, higher cortices and limbic systems to sit in seperate corners of the room and ignore each other for a bit once you reach doses of 1mg/kg.
The wonderful pain relief afforded by ketamine is thanks to agonism of the usual suspects - mu, kappa and delta opioid receptors.
How to give the ketamine
Doses
- The IV dose is 1 - 1.5 mg/kg and kicks in fairly reliably after 90 seconds or so
- The IM dose is 4 - 5 mg/kg* and takes at least 2 or 3 minutes to work
In general you'd choose IV wherever possible, as it's faster acting, faster to wear off and easier to titrate, but sometimes your hand is forced.
*Think about the concentration of your ketamine - if you're giving 5mg/kg IM to an adult then you'll want a higher concentration than 10mg/ml or that is going to be a very painful injection.
Side effects
- Emergence delirium
- Hypersalivation
You can offset the hypersalivation with atropine (20mcg/kg in children up to 600mcg), especially if you want a dry mouth or nose
Also, remember that young kids may need a higher relative dose due to their rapid metabolism and inexplicable ability to chew through anaesthetic drugs like a bored husky through a couch.
If you're worried about raised intracranial or intraocular pressure - this concern is largely unsubstantiated and shouldn't represent an absolute contraindication to using ketamine if it's the best agent available.
Behold the wonder of Ketofol
So propofol is good, and ketamine is good - why not both?
Ketamine provides the cardiovascular stability and analgesia without respiratory depression, and propofol smooths out the ups and the downs and also acts as an antiemetic.
It does add a little complexity, and you can run the risk of under- or overdosing as a result of giving two agents, but the general consensus is one of increasing support for ketofol when used by experienced hands.
As always, there is no perfect one agent (or mixture) - you should build experience with a technique and cocktail that works for you, and stick to your guns.
Some FRCA questions for fun
What doses of ketamine correspond to each level of sedation?
As a general rule, for IV administration:
- 0.5mg/kg = analgesia and light sedation
- 1mg/kg = procedural sedation
- 1.5-2mg/kg = dissociative anaesthesia
What are the benefits and disadvantages of ketamine for procedural sedation?
Benefits
- Maintenance of airway reflexes
- Cardiovascular stability (maintained blood pressure and heart rate)
- Maintained respiratory drive
- Bronchodilatation
- Analgesia
Disadvantages
- Technically there's a slightly increased risk of laryngospasm but it's rare
- Hypersalivation
- Not suitable for patients with poorly-managed psychosis
How long should patients be fasted prior to sedation?
Ideally you should be treating this in the same vein as a general anaesthetic:
- 6 hours for food
- 1-2 hours for clear fluid
But you are allowed to use clinical judgement at least once in a while - if you have a patient in agony who needs a joint popping back into place and they had a packet of crisps five and half hours ago - that's probably okay
Useful resources and further reading






