Ankylosing Spondylitis

It's hard to know what nuanced factual nuggets will be asked about in the written Final FRCA paper, so we've covered as many as possible here. For the purposes of the time-pressured SOE component we'd advise focusing on how you would safely anaesthetise the patient with ankylosing spondylitis, rather than the specific details of diagnosis and management of this multisystem disease.
As with many multisystem diseases, ankylosing spondylitis gets examined because it combines:
- Difficult airway management
- Difficult regional anaesthesia with neurological implications
- Restrictive respiratory physiology
- Cardiovascular instability
- Positioning and musculoskeletal risks
- Perioperative pharmacological management of DMARDs and immunosuppressants
All in one convenient package.
What is it?
Here's your exam headline for the viva:
Ankylosing spondylitis is a chronic, inflammatory, seronegative, spondyloarthropathy that primarily affects the axial skeleton and sacroiliac joints, but has multisystem implications for the anaesthetist.
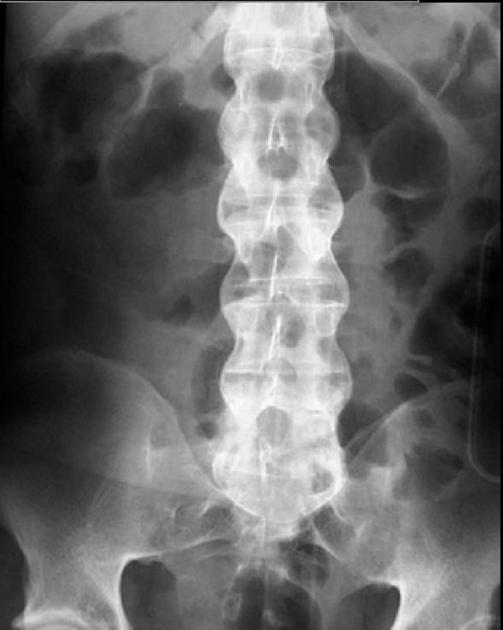
This chronic inflammation results in progressive spinal rigidity and ossification, causing the classic 'bamboo spine' which is simultaneously rigid and fragile, making your day as the anaesthetist somewhat more complicated.
How is ankylosing spondylitis diagnosed?
- Clinical and radiological criteria
- Rheumatoid factor is absent
- MRI can provide a radiological diagnosis
- Modified New York Criteria
Let's start with a classic final FRCA opening gambit question that's frustratingly broad and can trip you up if you don't start superficial enough.
What are your anaesthetic concerns for a patient with ankylosing spondylitis?
Ankylosing spondylitis is a multisystem autoimmune condition with multiple areas of concern for the anaesthetist including:
- Airway management
- Respiratory homeostasis
- Cardiovascular instability
- Positioning and neurological injury
- Pharmacological and physiological implications of comorbidity and immunosuppression
Each of which need to be addressed and optimised in turn.
By structuring your response like this, you invite the examiner to then dive further into one of your carefully selected sections, while reassuring them that you also understand the other system issues that they might not get time to ask you about.
Who gets it?
Classically it's young men with the HLA-B27 genotype, but that's hardly a rule.
- 2:1 male to female ratio
- Peak onset between 20 and 30 years of age
- Males have more spinal and pelvic involvement
- Females have greater wrist, knee and ankle disease
What causes it?
Short answer is we don't know, but probably a mixture of:
- Genetic predisposition - HLA-B27, TNF alpha etc
- Infectious triggers - viral/bacterial
- Other risk factors - age, gender, ethnicity
In terms of pathophysiology, there are two main hypotheses as to what is actually going on:
- Arthrogenic peptide hypothesis
- HLA-B27 folding hypothesis
I'd be amazed if you need to know it to any more detail than this, but it's feasible that it could be a particularly obscure CRQ answer.
Feel free to dive down a ChatGPT rabbit hole with them and see what you find.
Tell me about HLA-B27
Around 85% of patients with ankylosing spondylitis are positive for HLA-B27
- But it's not specific - only 5% of those with HLA-B27 get ankylosing spondylitis
It's not really clear what the significance of the allele's presence is, only that the examiners seem to like it.
Airway
As if airway management isn't already your primary concern for every patient, in ankylosing spondylitis there are a number of things to think about that can cause you trouble if you're not paying attention.