A recipe for Alfentanil TIVA

Remifentanil is useful but I have never liked it in cases where one is reliant on subsequent IV analgesia. The transition from a carefully titrated anaesthetic to smashing in 10mg morphine, or the like, towards the end has always irked me. You don’t really know where you are!
Most people use small aliquots of Alfentanil for short sedation cases but when given in larger amounts by infusion it can be used entirely differently. Below is a graph of CSHT’s which are relevant in this context.

I use this anaesthetic for cases longer than an hour for which I don’t use regional as the primary analgesia.
IMO one needs this long to infuse adequate Alfentanil and have enough time to get the patient breathing again.
Draw 5mg Alfentanil up to 50mls with normal Saline. (100mcg/ml)
Select the maitre model (freely available to download) on the Alaris PK pump which is generallt ubiquitous in the NHS.
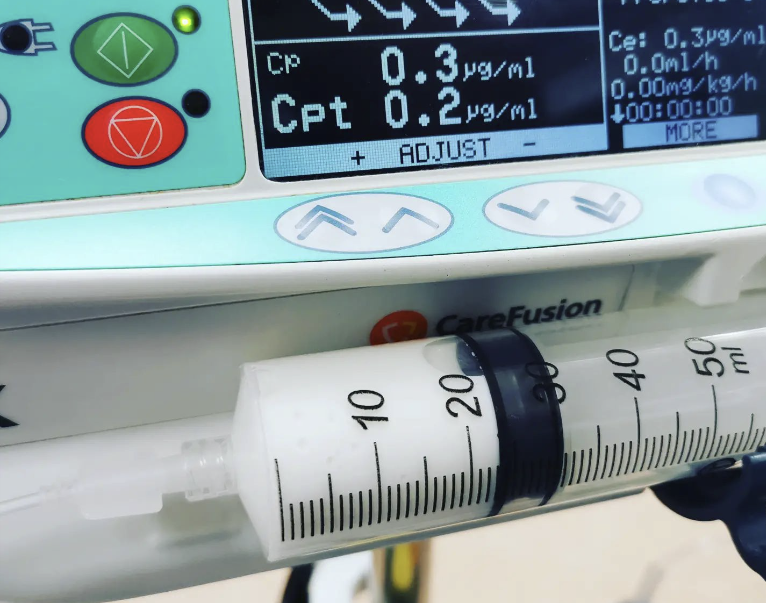
Select a Cpt of 120mcg/ml and wait for it to reach target Ce before starting the propofol.

This will administer a far larger and slower bolus than one would normally deliver at induction and result in a cardio stable therapeutic Ce. For an average man 120mcg/ml will be reached in 3 min and 2mg of drug.
I watch the patient closely at this point as the Ce at which they relax and then go apnoeic is useful in guesstimating at what level they are likely to start breathing again on emergence at the end. More about that later….
I then start the propofol. Marginally off piste, Guedel’s plains of anaesthesia are useful here and although slightly bastardised by modern practice I wait until the patients’ eyes are fixed in the midline before instrumenting the airway.
BIS is also useful.
I generally use this technique for larger cases, and because the patient will de facto be apnoiec at these Alf concentrations I usually intubate. Unless there is an airway issue I do not use muscle relaxant (I will write another thread about that if more than 2 people read this)
As soon as the tube is in I reduce the Cpt to about 90mcg/ml and leave it there for the duration of the case.

The very slight intricacy of this technique is towards the end. Patients will remain apnoeic until a Cpt between 60>x>70mcg/ml, so one has a set a decrement concentration. One does this by pushing the <?> key and entering a number of your choice.
I choose the decrement concentration depending on how the patient went off the sleep and how painful the operation was. Depending on habitus and length of surgery the decrement can be anything from 5 minutes to over an hour which is why using the model is vital.
The decrement time is set to 70mcg/ml in the below and is the lower right figure……14 mins. I have set the target Cpt to overshoot this in this instance.

Whilst the Alfentanil Cpt is decreasing I will decrease the MV to stimulate respiration. An ETCO2 of approx 7 is normally about right to do the latter without completely ruining the acid base balance and waking someone up feeling like they have a neck size of 30 inches!
When the patient resumes respiration I establish a regular pattern on PSVpro. Having done that, and if necessary, I then up titrate the alfentanil to a RR of about 8 to ensure maximal safe analgesia concentration on emergence.
No other analgesia is routinely required in theatre aside from the standard “non anaesthetic” affairs (ie paracetamol, NSAIDS). This can be, and often is, a 2 drug anaesthetic.
Every anaesthetist knows that there are hundreds of ways to safely skin a cat and giving someone else’s anaesthetic is almost impossible. That being said this is the best one I can give, I believe in it and have anaesthetised colleagues who subsequently agree!
Thanks for reading!
Originally tweeted by Luke (@Shr_Nottingham) on August 6, 2022.
Reproduced with Permission by Anaestheasier